Vaccines are one of the most remarkable medical inventions. They have eradicated two major infectious diseases: smallpox in humans and rinderpest in cattle1. Through vaccination programs worldwide, many children grow up healthy and free of debilitating diseases such as mumps, rubella, diphtheria, and tetanus. Since 2021, COVID-19 vaccines have enabled more and more people to carry on with their lives amid the pandemic.
The rapid development of several vaccines addressing the latest pandemic left many people understandably skeptical of the safety and reliability of COVID-19 vaccines. In a regular scenario, it would take 10 to 15 years to develop and approve a vaccine for use2. However, the emergency of the COVID-19 pandemic required fast action: the SARS-CoV-2 virus spread worldwide; hospitals were fully booked with infected people, and healthcare workers were under heavy pressure to take care of their patients and themselves. Meanwhile, the economy was also taking a toll on governments’ safety measures to keep the infection numbers as low as possible. Pharmaceutical companies and regulatory agencies needed to keep up and advance as fast as possible to guarantee that safe products would be available so that our lives would get back to normal as soon as possible.
Within one year, multiple vaccines were developed and authorized for emergency use. Several platforms were used to make the most promising candidate vaccines. Some were based on traditional approaches involving the whole virus (weakened or inactivated) or parts of it, such as fragments of a viral protein. Others were based on modern technology and used the virus’s genetic material, e.g., DNA or mRNA2.
How our bodies respond to a viral infection
Viruses are sneaky and clever tiny microbes. Basically, they need living cells to multiply. When a virus enters our bodies, it attaches to our cells and injects its genetic material. This material contains the recipe for our cells to make more copies of that virus. Our cells, then, become a factory of viruses that will infect more cells and repeat the process.
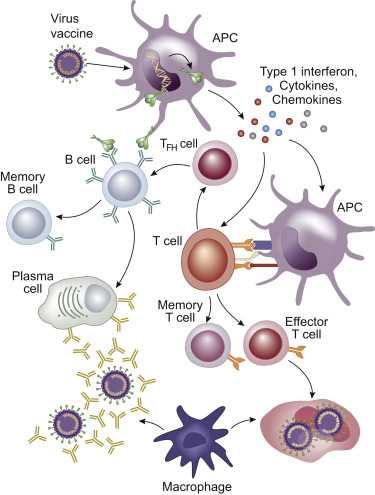
Luckily, our immune system recognizes any foreign material or organism. Once a foreign germ is identified, it is captured and processed by specific cells called “antigen presenting cells (APCs).” The APCs, then, bring fragments of the pathogen and expose them to T cells and, after that, the B cells produce little soldiers called antibodies. The antibodies attach themselves to the virus, preventing it from attacking more cells and marking it for destruction by other immune soldiers called macrophages, who will literally eat up the antibody-tagged virus and virus-infected cells. In parallel, certain cells develop a long-lasting memory3. By the time the virus enters in contact again with our cells, our immune system is ready to respond quickly.
However, it takes a few days for our immune system to learn how to defend our bodies. Therefore, vaccines are so important. They train our bodies to be ready before a virus, bacteria, or another pathogen enters our bodies. This training consists of presenting our immune system to the pathogen itself (either live-attenuated or inactivated) or parts of it, such as proteins or sections of the genetic material.
Debunking the myth of the danger of mRNA and DNA vaccines
Despite the COVID-19 vaccines’ benefits, many people got suspicious because of their fast development and prompt availability in several countries. Then, a scary myth became popular: people could turn into mutants when injected with mRNA or DNA vaccines. Having a virus’ genetic material inserted in our cells raised concerns that such material would take over our cells and mutations could happen.
The myth creators and supporters did not realize a few things. Foremost, and the most obvious reason not to be concerned, is that in every viral infection, the genetic material from the virus inevitably enters our bodies and cells. Yet, most viral infections do not cause the viral DNA to become part of our genome. There are exceptions, such as the infection caused by the human immunodeficiency virus (HIV), but coronavirus and influenza virus do not affect our cells in that way.
Second, our body has multiple mechanisms to destroy the genetic material after injection. One of them is led by APCs such as dendritic cells or macrophages. Another one is facilitated by both extracellular and intracellular enzymes such as RNAses and DNAses. After injection, part of the material is processed and degraded by APCs and enzymes. Another part is translated into proteins (e.g. spike protein of SARS-Cov-2) that will be recognized as foreign material which will initiate an immediate immune response4. The main mechanism behind the effectiveness of the mRNA vaccine is the activation of the B cells. Molecular interactions involving the spike protein and B cells result in memory B cells, which are responsible for memorizing foreign material4. If our bodies were a kitchen, our cells would be chefs that read the recipe and throw it away in the trashcan once the food is ready. After vaccination, memory B cells are ready to act once SARS-CoV-2 enters our body.
Finally, both DNA and mRNA are intrinsically unstable and prone to degradation due to the presence of RNAses and DNAses in the serum and plasma4. Studies show that they both are degraded within one week after the injection with a minor fraction remaining intact at the injection site5. In fact, during the vaccine preparation, few modifications have to be made to the mRNA structure to prevent degradation before it is recognized by the immune system4.
The benefits of mRNA vaccines in the fight against the COVID-19 pandemic are clear. They have enabled the rapid and versatile development of multiple vaccines with proven high protective efficacy4. If you want to stay healthy and strong and you’re not vaccinated yet, do yourself a favor. Train your immune system and protect your body against severe illness and hospitalization by getting your shot as soon as possible.
Despite the anti-vaxxers’ campaign, many developed countries are on track to recovering their normal life. In contrast, several low- and middle-income countries have not had the same luck. Many of these countries have not been able to get prompt vaccine supplies. Why does this matter? That is a story for another time.
References
- Greenwood B. The contribution of vaccination to global health: past, present and future. Philos Trans R Soc Lond B Biol Sci. 2014;369(1645):20130433. Published 2014 May 12. https://doi.org/10.1098/rstb.2013.0433
- William O. Hahn, Zanthia Wiley, COVID-19 Vaccines, Infectious Disease Clinics of North America, 2022, ISSN 0891-5520, https://doi.org/10.1016/j.idc.2022.01.008
- Khalil El Karoui, An S. De Vriese, COVID-19 in dialysis: clinical impact, immune response, prevention, and treatment, Kidney International, 2022, ISSN 0085-2538, https://doi.org/10.1016/j.kint.2022.01.022.
- Park JW, Lagniton PNP, Liu Y, Xu RH. mRNA vaccines for COVID-19: what, why and how. Int J Biol Sci. 2021;17(6):1446-1460. Published 2021 Apr 10. https://doi.org/10.7150/ijbs.59233
- Hobernik D, Bros M. DNA Vaccines-How Far From Clinical Use?. Int J Mol Sci. 2018;19(11):3605. Published 2018 Nov 15. https//doi.org/10.3390/ijms19113605