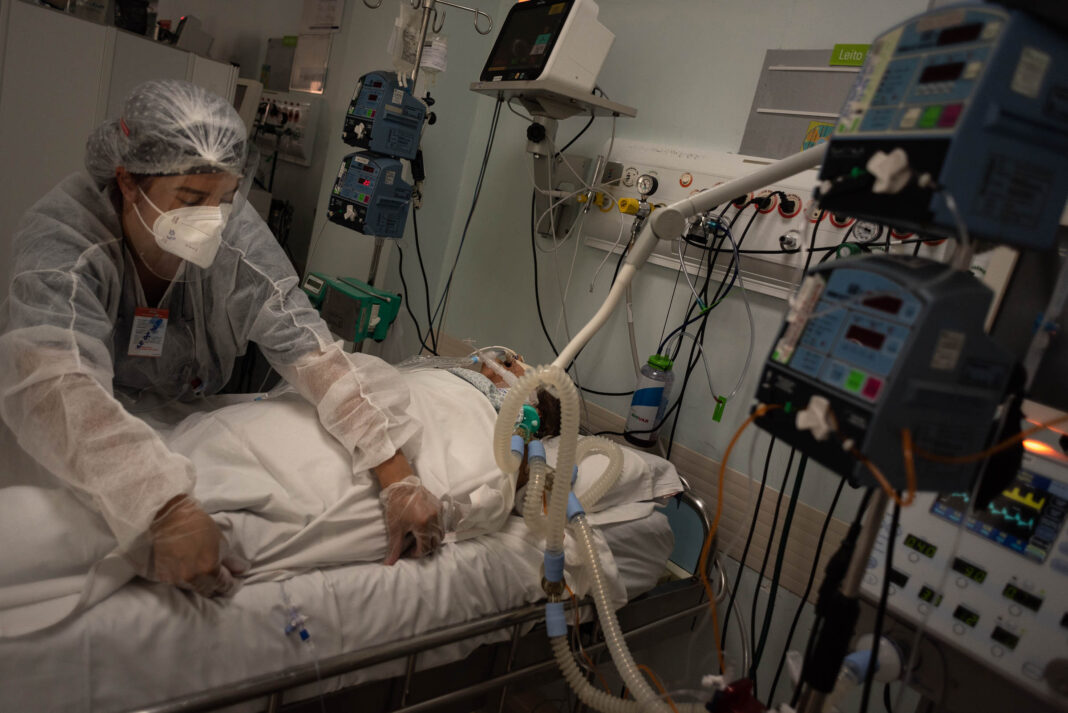
A recent study carried out in the UK concluded that people discharged from COVID-19 hospital admission had markedly higher risks for rehospitalization and death than the general population and people hospitalized with influenza.
Furthermore, the data showed that COVID-19 hospitalized patients were more likely to have baseline comorbidities than the general population. This reflects known associations between comorbidities and risks of severe COVID-19 effects.
The study followed up patients for up to ten months; it is the first analysis to give evidence about medium to long-term adverse outcomes following acute Coronavirus illness.
Due to the high rates of Coronavirus infection in many countries, this research aimed to help inform healthcare providers and raise awareness of potential complications for these patients. Additionally, the results could be useful with public health resources planning.
Researchers quantified the extent to which people who have been in hospital with COVID-19 may have higher chances of dying or being readmitted to the hospital; overall, or for specific illnesses. They compared these patients with people in the general population and people hospitalized with influenza.
The group of people from the general population were patients under follow-up in 2019. This group matched to the COVID-19 group on age (within three years), sex, and Sustainability and Transformation Plans (a geographical area used for the National Health Service administration – NHS). The rationale for matching to 2019 data was to provide a comparison with routine risks during pre-pandemic times. These people were hospitalized because of diverse health issues like Hypertension, Asthma, some immunosuppressive disease, organ dysfunction (kidney, liver) to name the most common comorbidities for this control group.
People who had a COVID-19 hospitalization were more than twice as likely to be hospitalized or die a week after discharge, with higher risks overall and for a range of specific causes than the general population.
Compared with influenza patients, people who got hospitalized for COVID-19 had a broadly similar or lower risk of several outcomes. However, the risk of death overall, readmissions or death due to the initial infection, and dementia death were higher for the latter.
The study, released last week on PLOS Medicine, is consistent with emerging evidence from early research suggesting that some people infected with SARS-CoV-2 can experience health problems for at least several months after the acute phase of their infection. Some afflictions are fatigue, pain, respiratory and cardiovascular symptoms, mental health problems, and cognitive disturbances. It has been frequently described as “post-acute COVID-19 syndrome”.
“Epidemiological characterization of such sequelae has been limited. The present study helps to contextualize these observations by adding explicit comparison with risks experienced by the general population and by people with a recent influenza hospitalization,” the scientific team argued.
The research was led by the Faculty of Epidemiology and Population Health at the London School of Hygiene and Tropical Medicine; and the DataLab from the Nuffield Department of Primary Care Health Sciences of the University of Oxford. The team suggested that all these consequences might be minimized or mitigated by increasing the monitoring of patients in the months following hospital discharge and getting greater awareness among patients and clinicians of potential problems.
COVID-19 patients were more likely than influenza patients to be readmitted or die
Researchers conducted a cohort study using linked primary care and hospital data in the OpenSAFELY platform. They compared risks of hospital admission and death, overall and by a specific cause, between people discharged from COVID-19 hospitalization with Coronavirus as the primary diagnosis—from February to December 2020—and surviving at least one week. This group was compared with demographically matched controls from the general population and people discharged from influenza hospitalization from 2017 to 2019.
The sample included 24,673 post-discharge COVID-19 patients, 123,362 general population controls and 16,058 influenza controls, followed for 315 days.
Most of the COVID-19 patients 66 years old on average, were male and of white ethnicity. The COVID-19 group was more likely to be obese and less likely to be current smokers than both comparison groups. Preexisting comorbidities were more common in COVID-19 and influenza-discharged patients than in general population controls. COVID-19 patients had a longer median duration of hospital stay and were more likely to have received critical care during their admission than influenza patients.
The overall risk of hospitalization or death was higher in the COVID-19 group than general population controls but slightly lower than influenza. All-cause mortality was higher in the COVID-19 than for the general population and the influenza control group.
Risks for cause-specific outcomes were higher in COVID-19 survivors than in general population controls and similar or lower in COVID-19 compared with influenza patients. However, COVID-19 patients were more likely than influenza patients to be readmitted or die due to their initial infection or other lower respiratory tract infection and to experience mental health or cognitive-related admission or death. Higher risk of dementia hospitalization or death particularly affected COVID-19 survivors with preexisting dementia. The scientific paper pointed out an excess of deaths for dementia as the underlying cause.
These findings suggest a need for services to support and closely monitor people following discharge from hospital with COVID-19, for example, through more frequent/active follow-up in primary care in the weeks and months following a hospitalization.
“Ongoing monitoring will be important to investigate whether these patterns persist in the light of new variants and increasing levels of vaccination,” the researchers concluded.
References
Bhaskaran, K., Rentsch, C. T., Hickman, G., Hulme, W. J., Schultze, A., Curtis, H. J., Wing, K., Warren-Gash, C., Tomlinson, L., Bates, C. J., Mathur, R., MacKenna, B., Mahalingasivam, V., Wong, A., Walker, A. J., Morton, C. E., Grint, D., Mehrkar, A., Eggo, R. M., . . . Goldacre, B. (2022). Overall and cause-specific hospitalisation and death after COVID-19 hospitalisation in England: A cohort study using linked primary care, secondary care, and death registration data in the OpenSAFELY platform. PLOS Medicine, 19(1), e1003871. https://doi.org/10.1371/journal.pmed.1003871
Nalbandian A, Sehgal K, Gupta A, Madhavan MV, McGroder C, Stevens JS, et al. Post-acute COVID-19 syndrome. Nat Med..2021; 27(4):601–15. https://doi.org/10.1038/s41591-021-01283-z PMID: 33753937.
Mazza MG, De Lorenzo R, Conte C, Poletti S, Vai B, Bollettini I, et al. Anxiety and depression in
COVID-19 survivors: Role of inflammatory and clinical predictors. Brain Behav Immun. 2020; 89:594–
600. https://doi.org/10.1016/j.bbi.2020.07.037 PMID: 32738287.
Xiong Q, Xu M, Li J, Liu Y, Zhang J, Xu Y, et al. Clinical sequelae of COVID-19 survivors in Wuhan,
China: a single-centre longitudinal study. Clin Microbiol Infect. 2021; 27(1):89–95. https://doi.org/10.
1016/j.cmi.2020.09.023 PMID: 32979574.