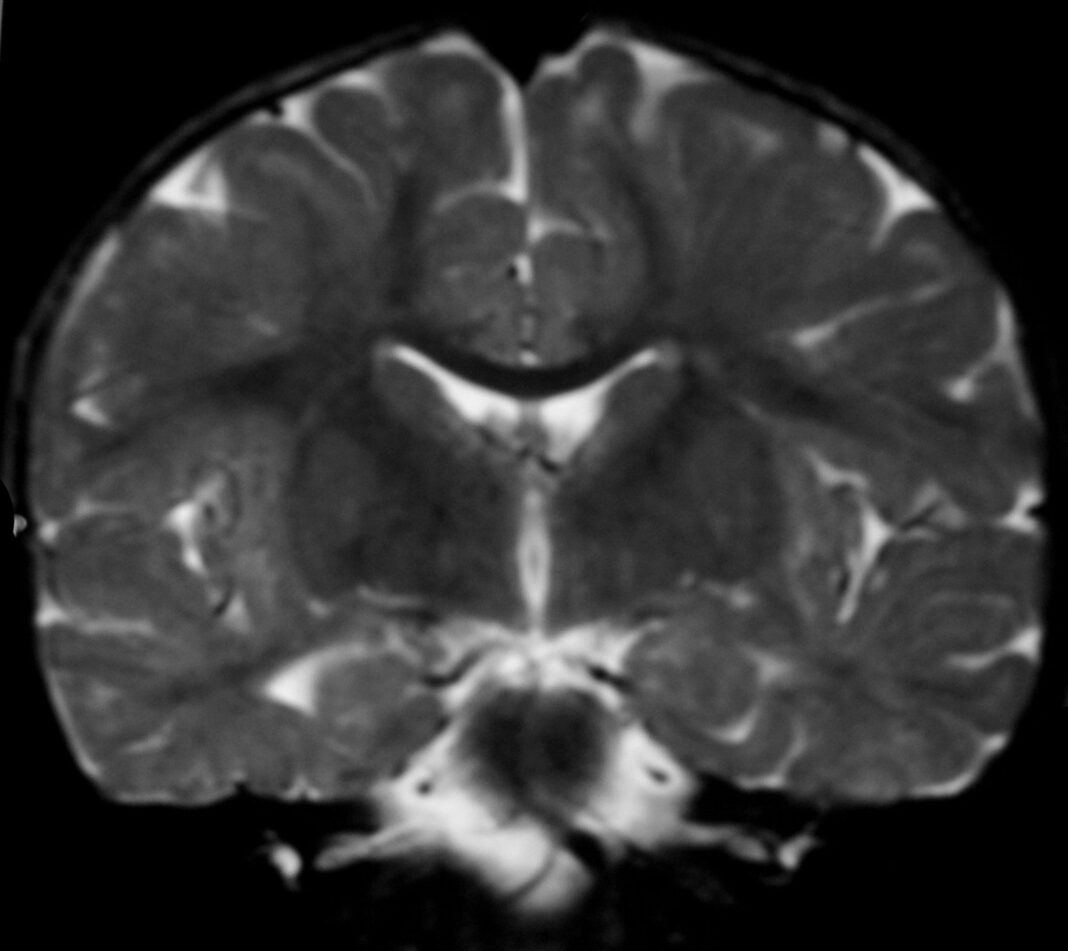
Alexander disease refers to a progressive disorder of cerebral white matter, commonly detected in infants and children. Its prevalence is unknown; however, approximately 500 cases have been reported since its first description in 1949. The neonatal form appears within the initial 30 days following birth and is characterized by gastrointestinal symptoms, neurologic symptoms, stiffness in legs and arms, seizures, intellectual disabilities, developmental delay, and usually death within two years.
Despite no current treatment, Tracy Hagemann and collaborators conducted a new study at the University of Wisconsin-Madison using a rat model of this disease to develop a prospective treatment for the characteristically fatal disorder.
According to Hagemann, Alexander disease generally involves the disintegration of the brain’s white matter, frequently remaining undiagnosed until the appearance of pronounced symptoms. A characteristic feature of this disease is the development of Rosenthal fibers, which are abnormal protein aggregates generated by a mutation in the GFAP gene that produces glial fibrillary acidic proteins.
Hagemann and collaborators had developed a mouse model three years ago to demonstrate the role of antisense oligonucleotides in eliminating Rosenthal fibers and lessening GFAP. Oligonucleotides are short polymers made up of single- or double-stranded RNA or DNA molecules used for the management or treatment of numerous diseases.
Nonetheless, mice exhibit few symptoms of Alexander disease, thus making it difficult to assess the significant impact of the treatment on the quality of life or behavior. Clinicians usually consider Alexander disease an uncommon genetic disorder that affects the brain’s white matter. This clinical phenomenon was not observed in the mouse model. Therefore, rats were considered a better choice for a preclinical model.
The researchers created a rat model that could reflect the damage of the white matter and associated physical symptoms observed in patients. The model provided better opportunities to assess symptom improvement in response to antisense oligonucleotide treatment, i.e., oligonucleotides containing complementary sequences. The model displayed myelin damage, high accumulation of GFAP, extensive formation of Rosenthal fibers all over the spinal cord and brain, high death rate, and motor injury.
It was difficult to discriminate against rats that underwent antisense oligonucleotide treatment before developing key physical symptoms from their healthy complements. After beginning the treatment, severely affected rats displayed extreme improvement in symptoms and showed a reversal of white matter damage.
Hagemann mentioned that antisense oligonucleotides work by removing the Rosenthal fibers, preventing the disease onset at an early stage. Moreover, this treatment can reverse the disease makeup at a later stage.
The findings of this study should be credited to the far-reaching research by Messing on Alexander disease conducted over the previous two decades. Besides paving the groundwork for human trials, the animal model showed the approach to discover several facets of Alexander disease that are unclear, together with the novel prospect to explore the association between white matter damage and GFAP mutations in mammals.
References
Hagemann, T. L., Powers, B., Lin, N. H., Mohamed, A. F., Dague, K. L., Hannah, S. C., … & Messing, A. (2021). Antisense therapy in a rat model of Alexander disease reverses GFAP pathology, white matter deficits, and motor impairment. Science Translational Medicine, 13(620), eabg4711. http://www.science.org/doi/10.1126/scitranslmed.abg4711
Srivastava, S., Waldman, A., & Naidu, S. (2020). Alexander disease. PMID: 20301351
Yoshida, T., Sasaki, M., Yoshida, M., Namekawa, M., Okamoto, Y., Tsujino, S., … & Nakagawa, M. (2011). Nationwide survey of Alexander disease in Japan and proposed new guidelines for diagnosis. Journal of neurology, 258(11), 1998-2008. https://doi.org/10.1007/s00415-011-6056-3
Prust, M., Wang, J., Morizono, H., Messing, A., Brenner, M., Gordon, E., … & Vanderver, A. (2011). GFAP mutations, age at onset, and clinical subtypes in Alexander disease. Neurology, 77(13), 1287-1294. https://doi.org/10.1212/WNL.0b013e3182309f72
Messing, A., Brenner, M., Feany, M. B., Nedergaard, M., & Goldman, J. E. (2012). Alexander disease. Journal of Neuroscience, 32(15), 5017-5023. https://doi.org/10.1523/JNEUROSCI.5384-11.2012
Hagemann, T. L., Powers, B., Mazur, C., Kim, A., Wheeler, S., Hung, G., … & Messing, A. (2018). Antisense suppression of glial fibrillary acidic protein as a treatment for Alexander disease. Annals of neurology, 83(1), 27-39. https://doi.org/10.1002/ana.25118